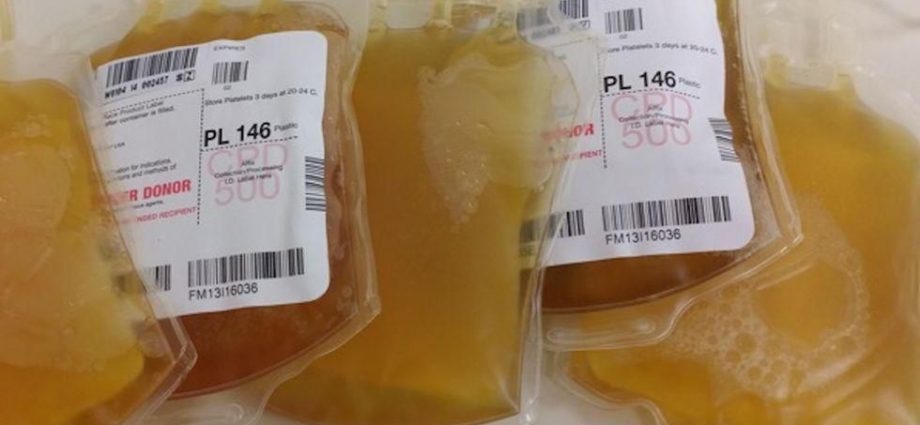
FRIDAY, Aug. 20, 2021 (HealthDay News) — Early treatment with COVID-19 survivors’ blood plasma doesn’t prevent disease progression in people who have mild COVID-19 symptoms but are at risk for more severe illness, a new clinical trial finds.
“As physicians, we wanted this to make a big difference in reducing severe illness and it did not,” said principal investigator Dr. Clifton Callaway, professor of emergency medicine at the University of Pittsburgh.
Last year, the U.S. Food and Drug Administration gave emergency use authorization for survivors’ (“convalescent”) plasma to be given to hospitalized COVID-19 patients.
Researchers wondered whether convalescent plasma might also benefit patients who were recently infected with SARS-CoV-2 but were not seriously ill and could be treated as outpatients. The aim: to head off progression to severe illness.
The study — largely funded by the U.S. government — began in August 2020. It included more than 500 patients from 48 emergency departments across the United States. Patients’ median age was 54, meaning half were older, half younger.
Each had at least one risk factor for progression to severe COVID-19, such as obesity, high blood pressure, diabetes, heart disease or chronic lung disease.
Participants were randomly assigned to receive either high-titer convalescent plasma containing anti-COVID antibodies or a placebo.
The trial was stopped in February, because results to that point found the convalescent plasma treatment was ineffective.
Within 15 days of treatment, disease progressed in 30% of the plasma group and 31.9% of those in the placebo group. The findings were published online Aug. 18 in the New England Journal of Medicine.
“We were hoping that the use of COVID-19 convalescent plasma would achieve at least a 10% reduction in disease progression in this group, but instead the reduction we observed was less than 2%,” Callaway said in a news release from the U.S. National Institutes of Health. “That was surprising to us.”
It’s not clear why convalescent plasma treatment was ineffective, and Callaway said researchers are looking for possible explanations, including insufficient dose, treatment timing and patient-related factors.
According to study co-author Dr. Nahed El Kassar, “The results show that convalescent plasma does not appear to benefit this particular group. But the findings answer an important clinical question and may help bring researchers a step closer to finding more effective treatments against this devastating disease.”
El Kassar is medical officer at the U.S. National Heart, Lung, and Blood Institute (NHLBI).
Other studies of COVID-19 convalescent plasma are ongoing or are planned in different groups of people. They include one in outpatients who are recovering at home and another in individuals with high risk of exposure to COVID-19 to see if plasma can prevent infection.
Dr. Simone Glynn, chief of the NHLBI’s Blood Epidemiology and Clinical Therapeutics branch, is coordinating the trial. She said, “We need the results of these other convalescent plasma studies to get a clearer, more conclusive picture of its value for future treatments of COVID-19.”
More information
The U.S. Food and Drug Administration has more on convalescent plasma and COVID-19.
SOURCE: U.S. National Institutes of Health, news release, Aug. 18, 2021
Copyright © 2026 HealthDay. All rights reserved.